How to Treat Heel Pain

Heel pain can be surprisingly disruptive. What may begin as a mild discomfort can quickly develop into something that affects how you walk, exercise, and go about your day. Many people find themselves adjusting their routine, avoiding certain activities, or simply pushing through the pain, often without understanding why it has developed. Over time, this can begin to affect not just your mobility, but your overall quality of life.
If you’ve been wondering why your heel is so painful or looking for ways to treat it, understanding the cause is the first step towards lasting relief. At
Tennant Podiatry, we see heel pain all too often in patients, and although we understand the urge to treat it at home, we have seen time and again that the only way to truly rectify the impact it has on someone’s life is to identify the cause and create an ongoing, attainable treatment plan informed by medical professionals. So, what should you do if you are experiencing heel pain and how can we work together to treat it? We’ll start by explaining why it happens:
Why are heels vulnerable to pain?
Your heels absorb a significant amount of pressure every day. With every step, they take the impact of your body weight, acting as a natural shock absorber.
This constant load makes the heel particularly vulnerable to strain, especially when combined with:
- Long periods of standing or walking
- Sudden increases in activity or exercise
- Hard surfaces underfoot
- Unsupportive footwear
- Tight calf muscles or reduced flexibility
What causes heel pain?
It’s important to understand that heel pain is usually the result of irritation or strain within the soft tissues of the foot and in many cases, it develops from a combination of factors, rather than a single identifiable cause.
The most common causes include:
Plantar fasciitis (plantar heel pain): This is the most frequent cause of heel pain. It involves irritation of the plantar fascia, a thick band of tissue that supports the arch of your foot. Pain is often felt under the heel and may be worse in the morning or after rest.
Achilles tendon issues: Pain at the back of the heel is often linked to the Achilles tendon. This can become irritated due to overuse, tight calf muscles, or increased activity.
Heel bursitis: Inflammation of the small fluid filled sacs that cushion the heel can cause tenderness and discomfort, particularly when pressure is applied.
Heel spurs: These are small bony growths that may develop over time due to repeated strain. While not always painful themselves, they are often associated with long term stress on the foot.
Sudden increases in activity or load: A change in routine, such as starting a new exercise programme, walking more than usual, or returning to activity after rest, can overload the tissues before they have adapted.
Why do I have heel pain?
It’s very common for patients to believe that heel pain has emerged without reason, but the underlying cause is often unclear rather than unidentifiable. Heel pain, unless caused by an injury, is unlikely to appear suddenly. It develops gradually due to everyday habits and physical patterns that place repeated strain on the foot.
What we have found is that correct foot care is rarely taught and small acts of neglect build up over time, through no fault of your own. But once you identify foot and heel pain, it is vital to identify any ongoing activity that could be contributing and correct it.
You may be more likely to experience heel pain if you:
- Spend long periods standing or walking, particularly on hard surfaces
- Wear footwear that lacks support or structure
- Have tight calf muscles, which increase tension through the heel
- Have a walking pattern (gait) that places uneven pressure on the foot
- Have recently increased your level of physical activity
- Are carrying additional weight, increasing load through the heel
- Have reduced flexibility or strength in the lower limbs
What is plantar fasciitis?
Plantar fasciitis, sometimes referred to as plantar heel pain, is the most common cause of heel pain. It occurs when the plantar fascia, a thick band of tissue that runs along the sole of your foot, becomes irritated or overloaded.
This tissue plays an important role in supporting your arch and absorbing shock when you walk. However, when it is placed under repeated strain, small areas of stress can develop, leading to pain and stiffness.
People with plantar fasciitis often notice:
- Pain under the heel, particularly when taking the first steps in the morning
- Discomfort after periods of rest
- Pain that eases slightly with movement but may return later in the day
- Tenderness when pressing the underside of the heel
Despite the name, it is not always a case of inflammation. In many cases, it is related to degeneration from repeated strain, which is why rest alone does not always resolve the issue.
How to reduce heel pain
If you’re looking for ways to reduce heel pain, early self care can help ease symptoms and prevent further irritation while you wait for your appointment with a podiatrist.
Begin by:
Reducing strain on the heel:
Avoid activities that worsen pain, particularly high impact exercise or prolonged standing where possible.
Applying ice to the affected area: Cold therapy can help calm inflammation and provide short term relief when used regularly.
Wearing supportive, well cushioned footwear: Shoes that properly support your arch and absorb impact can significantly reduce pressure on the heel.
Using insoles or heel cushioning: These can help redistribute pressure more evenly across the foot.
Avoiding walking barefoot: Hard surfaces can increase strain on already sensitive tissues.
Incorporating gentle stretching: Stretching the calf muscles and plantar fascia can help relieve tension and improve flexibility over time.
How to treat heel pain properly
When considering how to treat heel pain, the most important factor is ensuring that treatment is appropriate for the underlying cause. What works for one person may not work for another, particularly if the source of pain differs.
Without addressing the underlying cause, symptoms may settle temporarily but are more likely to return.
Effective treatment typically involves:
- A clear diagnosis: Understanding whether the pain is coming from the plantar fascia, Achilles tendon, or another structure is essential for choosing the right approach.
- Reducing excessive load: This may involve temporary changes to activity levels, footwear, or daily habits.
- Improving foot function: Targeted exercises and support can help the foot move more efficiently and reduce strain.
- Correcting biomechanical issues: In some cases, orthotics or gait advice may be recommended to improve how pressure is distributed.
- Ongoing management where needed: Persistent or recurring heel pain may require structured treatment to fully resolve.
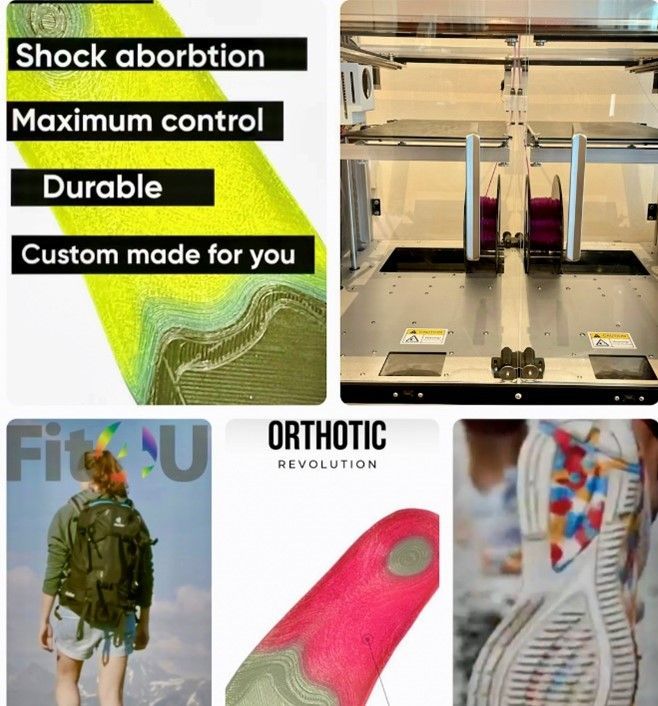
How can 3D custom orthotics help heel pain?
When heel pain is linked to how your foot moves or bears weight, providing the right support can make a significant difference. 3D custom orthotics are designed specifically for your feet, based on a detailed assessment of your gait and pressure distribution.
They work by:
- Redistributing pressure away from the painful area of the heel
- Supporting the arch, reducing strain on the plantar fascia
- Improving alignment, helping the foot function more efficiently
- Absorbing shock, reducing impact with each step
Unlike generic insoles, custom orthotics are tailored to you. This means they not only help relieve current symptoms but also address the underlying mechanical factors contributing to your heel pain.
How long is recovery for heel pain?
One of the most common concerns is how long heel pain will take to improve. Recovery can vary depending on the cause, severity, and how early treatment begins.
Mild cases may begin to improve within a few weeks with the right care but more persistent heel pain can take several months to fully settle. Longstanding or untreated pain may take longer and require more structured support. An experienced podiatrist will be able to assess the condition of your feet and provide you with a treatment plan that will give you more clarity on your healing timeline.
Is heel pain something you just have to live with?
There is a common belief that heel pain is simply part of getting older, being active, or spending long hours on your feet. In reality, this is rarely the case.
Heel pain is not something you should ignore or accept nor is it a normal part of ageing. Rest alone is often not enough to resolve the cause.
Most heel pain responds well to the right approach, particularly when it is assessed early and managed appropriately. If something doesn’t feel right, it is always worth having it checked. Addressing the issue sooner can make recovery simpler and more effective.
Why accurate diagnosis is essential for heel pain
Heel pain can feel similar regardless of the cause, but the underlying problem can vary significantly.
For example, pain under the heel may be linked to plantar fasciitis, while pain at the back of the heel may involve the Achilles tendon. Although the symptoms can overlap, the treatment approach for each is different.
Without a clear diagnosis, it is easy to use treatments that are not appropriate for your condition and delay recovery by focusing on the wrong area. A podiatrist will assess not only where the pain is, but why it has developed. This allows for effective treatment that is targeted and designed to prevent the problem from returning.
Take the first step towards lasting heel pain relief
Heel pain can affect every step you take, but with the right approach, it is often very manageable and, in many cases, fully treatable. If your symptoms are persisting, returning, or beginning to interfere with daily life, seeking professional advice can help you understand the cause and access the most effective treatment so you can return to doing the things that bring you joy without pain.
At
Tennant Podiatry, our accredited podiatrists treat all foot troubles and lower limb conditions with access to state of the art facilities and a comprehensive understanding of how feet are interconnected with the rest of the body. We provide
heel pain treatment with custom printed 3D orthotics designed to provide support, cushioning, and proper alignment to the foot, helping to alleviate pain and strain on the inflamed plantar fascia.
Our aim is always to make your life more comfortable through bespoke, informed treatment.
Contact us today.